The sedation may alleviate the awake intubation, but it requires conscientious administration and continuous monitoring as it can lead to airway obstruction and hypoxemia, while inadequate sedation could lead to discomfort, anxiety and excessive sympathetic discharge.ĭifferent pharmacological approaches have been reported to obtain conscious sedation and prevent cardiovascular changes during AFOI such as local anesthetics, benzodiazepines, opioids, α2 adrenoceptor agonists and less commonly propofol or ketamine. When AFOI is effectuated without sedation, it is commonly related to patient discomfort and severe hemodynamic responses, inducing catecholamine release by sympathetic stimulation, sympathetic stimulation, which may result in increased heart rate and blood pressure, arrhythmia, and cause myocardial ischemia and infarction in patients with risk factors, such as hypertension and ischemic heart disease. Proper local anesthesia also seems to reduce sedation doses of midazolam and fentanyl. During AFOI, coughing and laryngospasm in reaction to intubation can be problematic, so an effective airway local anesthesia is mandatory for the comfort of the patient and subsequent success of the procedure. 
This methodology could be conducted in totally awake patients after airway local anesthesia, under conscious sedation or by combining both approaches to limit airways reactivity. Īwake Fiberoptic Intubation (AFOI) is considered the Gold Standard in patients with a predicted difficult airway. Up to 30% of all deaths attributable to anesthesia are related to difficult airway management. Retrospectively registered 25 November 2014.Ĭombination drug therapy Deep sedation Dexmedetomidine Propofol.The estimated incidence of patients with difficult airway during clinical anesthesia is 1-18% in these patients with a difficult airway, the anatomy is frequently different from normal, and the inadequate airways management may result in hypoxemia, hypoventilation, aspiration, brain damage or even death. Additionally, it led to a similar onset time of propofol and achieved higher satisfaction scores. The combined use of propofol and dexmedetomidine provided cardiovascular stability with decreased adverse effects. Onset time was significantly longer in the D group (p < 0.001). 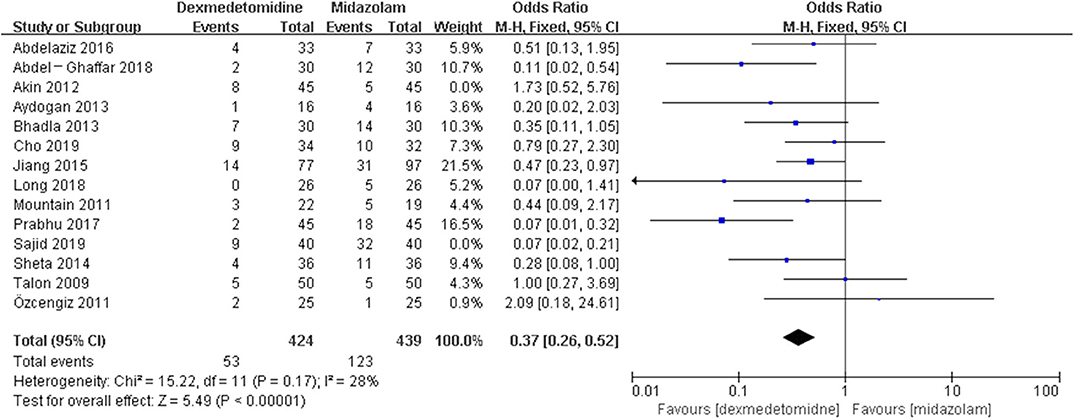
The satisfaction scores of the patients (p = 0.007) and surgeon (p < 0.001) were higher in the M group. The P group had higher incidences of hypoxia (p = 0.001), spontaneous movement (p < 0.001) and agitation (p = 0.001). The M group had a significant lower incidence of airway obstruction (p < 0.001) and the D group had a higher incidence of bradycardia requiring atropine (p = 0.001). The significantly higher mean arterial pressure (mmHg) in the D group and a significantly higher heart rate (beat/min) in the P group were observed. Cardiorespiratory variables, adverse effects, and drug efficacy were observed. The maintenance dose was adjusted to maintain an Observer Assessment of Alertness/Sedation score of 3. The M group received a half-dose of both drugs simultaneously. Therefore, we performed this randomized controlled trial to evaluate the combined use of propofol and dexmedetomidine.Įighty-seven adult patients undergoing hand surgery under brachial plexus block were randomly allocated to receive 1.6 μg/ml of the target effect site concentration of propofol (P group) and infusion of 0.4 μg/kg/h dexmedetomidine following a loading dose of 1.0 μg/kg for 10 min (D group). Although propofol and dexmedetomidine have been widely used for monitored anesthesia care, their adverse effects necessitate the search for better methods. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
